
What Is Lymphedema?
Lymphedema is a progressive yet manageable disease. As many as 10 million Americans live with this condition which affects the lymphatic system. The lymphatic system consists of lymph vessels and lymph nodes dispersed throughout the human body. It is responsible for collecting and removing lymph fluid (waste products from cells and tissues) from the skin transporting them eventually back to the venous system to maintain a fluid balance.
If the lymphatic system is damaged, an accumulation of lymphatic fluid over time may create progressive swelling, skin changes, ulcerations, & further complications if not adequately treated.
What Are The Causes?
Lymphedema can occur from malformations of the lymphatic system (primary) or from an injury caused by surgery, infection, malignancy, or trauma to the lymphatic system (secondary). In the United States, the most common type of lymphedema is due to surgery and radiation (secondary) treatment for malignancies (eg, breast cancer). Also, consider that if you develop an infection or have long-standing venous problems in your leg(s) (with or without ulcers present), secondary lymphedema may develop.
What is the treatment?
Lymphatic treatment may vary based on the condition, presentation, and severity of the involved area(s). Whether treating lymphatic dysfunction or Lymphedema, treatment may include, but not be limited to, an assessment of the involved area, manual lymphatic drainage, skin care, compression including bandages or garments, exercises, education, and/or adjunctive devices. The gold standard for treating Lymphedema is Complete Decongestive Therapy, including the treatment components described above.
Benefits of Lymphatic Treatment
The benefits of lymphatic treatment may include decreasing swelling, decreasing pain, rerouting lymphatic fluid from the swollen area to a healthy area, promoting lymph fluid reabsorption, improving venous return, optimizing the muscle pump effect, softening fibrotic tissue (hardened tissue from prolonged untreated swelling), improving joint range of motion & mobility while educating each patient on how to manage this condition.

MEET FRANK AVILES, JR.
Frank has been practicing as a physical therapist since 1991 dedicating his career to wound healing, lymphatic dysfunction, and patient advocacy. His experience, across the continuum of care, led to educating in academia, national, and international levels. He is a certified lymphedema therapist with national certification through the Lymphology Association of North America (LANA). In addition, Advance Lymphedema Management (ALM) designation, board Certified Wound Specialist (CWS), a fellow of the American College of Certified Wound Specialists (FACCWS), Advanced Wound Care Certified (AWCC), board member for the American Professional Wound Care Association (APWCA). He has also received the designation of Master for APWCA, is a board member for the Lighthouse Lymphedema Network, and serves as President for The Save a Leg Save a Life foundation.
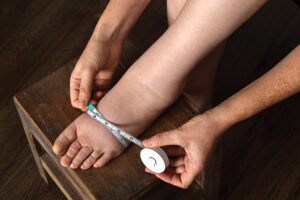
What Are The Symptoms?
Although there are multiple diagnostic tests available, lymphedema is typically diagnosed clinically by conducting a thorough patient history and evaluation.
Symptoms Include:
- Swelling in leg(s) and/or arm(s). The trunk and genitals can be involved as well.
- If both extremities are involved, one will be larger than the other.
- Severity of swelling may differ depending on onset. Initially, the swelling may be mild, but it can progress to severe.
- Skin may increase in redness, and infections are common.
- Skin may become hardened over time.
- Clothing or jewelry may become tighter on the affected body part.
- A decrease in mobility and flexibility of the affected body part may occur.
- Body part may feel heavy or uncomfortable.
Living With Lymphedema
Currently, there is no cure for lymphedema, so education is essential. Remember that once you have any type of surgery involving the removal or radiation of lymph nodes, you are at risk for developing lymphedema, whether the swelling develops immediately after surgery or years later. Early recognition followed by proper management leads to better outcomes. Treatment is aimed at moving lymph fluid using a multicomponent approach to decongest the involved body part. Ultimately, the patient assumes responsibility for his or her care. When fluid accumulates in an extremity, it can impact quality of life and the ability to perform activities of daily living (ADLs). Initially, it may seem that this swelling is a normal, self-limiting process; however, heaviness, stiffness, discomfort, and an increasingly swollen limb persists with time. Swelling may be reduced in the morning and increased by the evening. It is even possible to find unresolved swelling after sustaining a minor injury to the limb. ADLs such as combing your hair, picking up kids or objects, getting in and out of bed, and wearing normal clothing can become challenging and difficult. If not properly treated, patients may experience frequent skin infections. Any injuries or infection to the involved extremity will exacerbate this condition and lead to additional skin changes.
Treatment will be a lifelong process; however, it is manageable! Flare-up and exacerbations may occur: therefore, it is important to stay in contact with your healthcare provider(s) and report any changes or concerns promptly. Compression garments, either off the shelf or custom-made, will be used during the day. These garments have different levels of compression, and your healthcare provider(s) will assist you with the right compression level. If there are issues with wearing the appropriate level, alternative bandages are available, but this is prescribed on an individual basis based on your activity level, ability to apply/remove, and caregiver assistance. At night, short stretch bandaging or alternative devices may be prescribed instead of garments. Seek the advice from an expert, as not all garments are made equal.
Self-Care At Home
AVOID
- Skin injuries
- Insect bites
- Sunburns
- Strenuous exercise
- Tight clothing and jewelry
- Heating pads, hot showers
- Blood pressure and needle sticks on involved extremity
DO
- Maintain a low-salt, low-fat diet
- Drink plenty of liquids, especially water
- Take proper care of bandages and garments
- Elevate the involved extremity throughout the day
- Exercises while wearing compression
- Monitor your skin for injury and signs of infection
- Wear compression device when traveling
The Healing Power of Hyperbaric Medicine
HBOT helps white blood cells kill bacteria, and help osteoclast clean up the dead and infected bone. Once the infection is under control and all the dead bone is gone, new bone is laid down by osteoclasts. These processes require high levels of oxygen to function optimally. HBOT also helps antibiotics work better, and in conjunction with some antibiotics, helps eradicate the biofilms that form in many of these cases.
Increases White Blood Cell Effectiveness
Stimulates Release of Stem Cells
Improves Quality of Life in Patients
Most Conditions Covered by Insurance
How Long Does a Hyperbaric Treatment Take?
Most HBOT treatments generally take about 2 hours. Treatments for some indications can last up to 4 hours. Serious diving injuries can require a treatment for longer than 5 hours. The hyperbaric physician will determine how long each patient’s HBOT treatment will last.
Does Insurance Cover Hyperbaric Treatments?
Yes
Coverage for HBO is dependent on your insurance company’s Coverage Determination Policy.
No
Some indications are still not covered or coverage can vary by insurance provider. Contact us to verify coverage.
How Do I Get Treatment?
Patients can be referred to us by their physicians or call us for a consultation. While patients are undergoing treatment, they remain under the care of the referring physician, who will receive copies of the patient’s treatment documentation. In addition, out-of-area patients may be referred to an appropriate local physician at the discretion of the referring physician. To refer a patient, contact us at 678-388-9511, or download our referral form here.

Get help today! Contact our Cumming office.

Cumming, GA
1505 Northside Boulevard, Suite 1300, Cumming, GA 30041
Phone: 770-771-6400
Fax: 678-455-1969